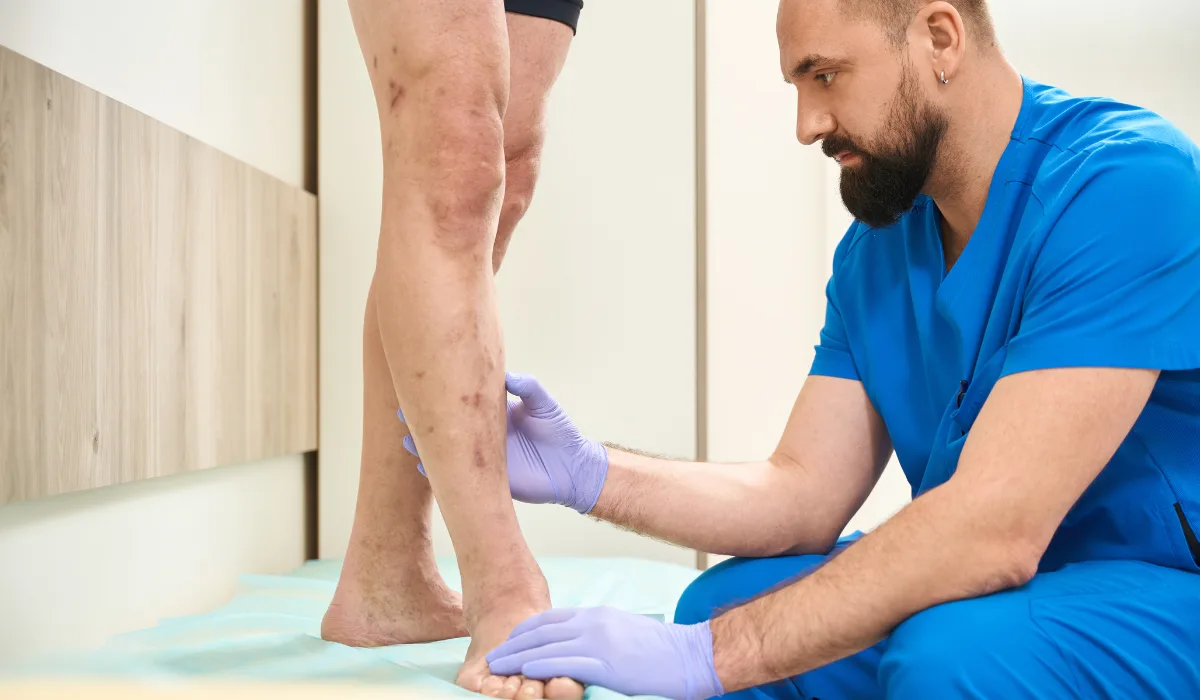
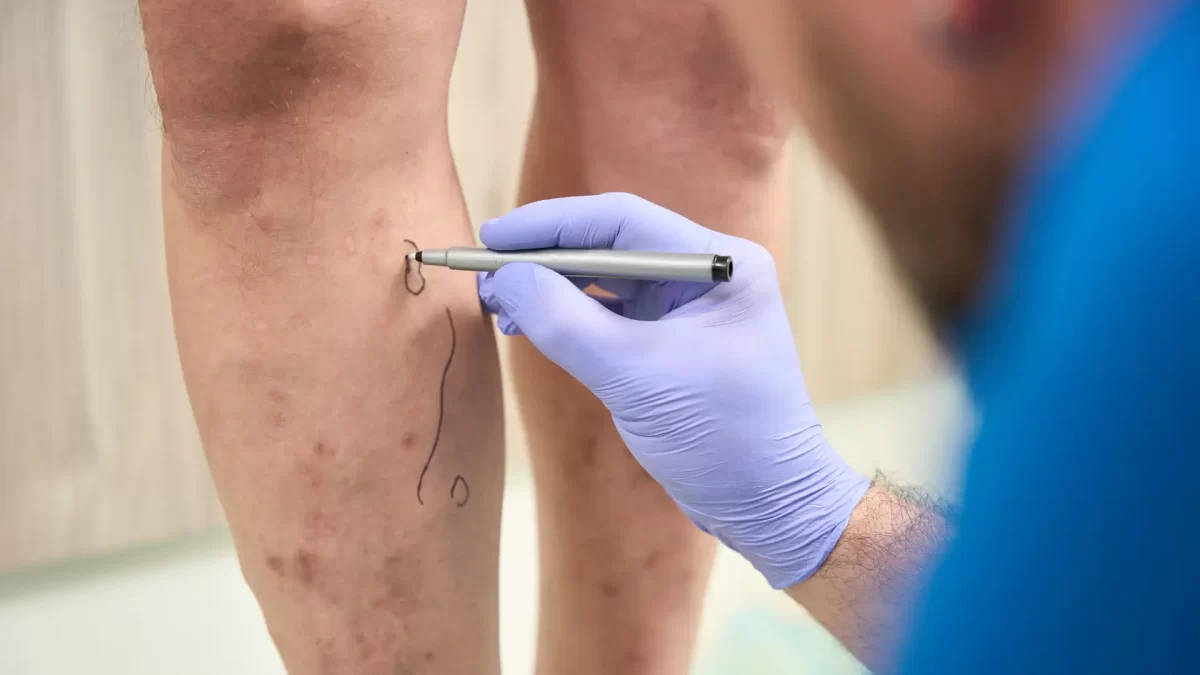
Varicose veins may seem like a minor concern at first, but can cause pain, discomfort, and other symptoms as they progress. These are normal veins that have enlarged, twisted, or overfilled with blood.
It happens when the tiny valves inside the veins weaken or fail and start to pool blood. They often appear blue or purple and are the most visible after prolonged periods of standing or sitting down.
When are varicose veins a problem?
If you experience any of the following, it’s time to take action:
- Persistent Pain or Heaviness
- Swelling in the Legs or Ankles
- Skin or Texture Changes
- Itching
- Bleeding or Ulcers
- Hardened Vein
- Severe Leg Pain (seek immediate medical help)
These symptoms suggest chronic venous insufficiency (CVI), a condition that worsens over time without medical intervention.
What are the risk factors?
Some people have a higher likelihood of developing varicose veins and its complications. If any of these apply to you, pay extra attention to your symptoms:
- Family history of varicose veins
- Job that requires long hours of sitting in one place
- Pregnancy; increased blood volume can weaken vein walls
- Obesity
- Age; veins lose elasticity as you age
- History of blood clots
Best ways to prevent varicose veins from progressing
The following steps can help you slow down progression and improve circulation. Here’s what you can do:
Keep Moving
Never sit in one position for more than 30 minutes. Spend 30 to 60 minutes every day to walk outdoors to ensure proper blood circulation. Do not cross your legs while sitting as it works prohibitively.

Elevate Your Legs
Make it a habit to prop your legs above heart level for 30 minutes every night. Even when sleeping, use a firm pillow to keep your legs elevated.
Use Compression Socks Daily
Compression socks apply gentle pressure on your legs to improve blood flow. They range from mild to firm, so you can level up as you get more comfortable with them. It’s also advised to wear them during long flights, road trips, or for extended periods of standing.
Work on Your Diet
Flavonoid-rich foods like citrus fruits, onions, and dark chocolate to reduce inflammation. Design a diet that includes these foods along with fibre and antibiotics. Lower salt intake, unless advised by your doctor, to prevent water retention.
Avoid Excessive Heat Exposure
Hot baths, sauna, steam, or sunbathing tend to dilate veins and worsen varicose veins. If your legs are swollen, soothe them with cool or room temperature water.
When to See a Doctor
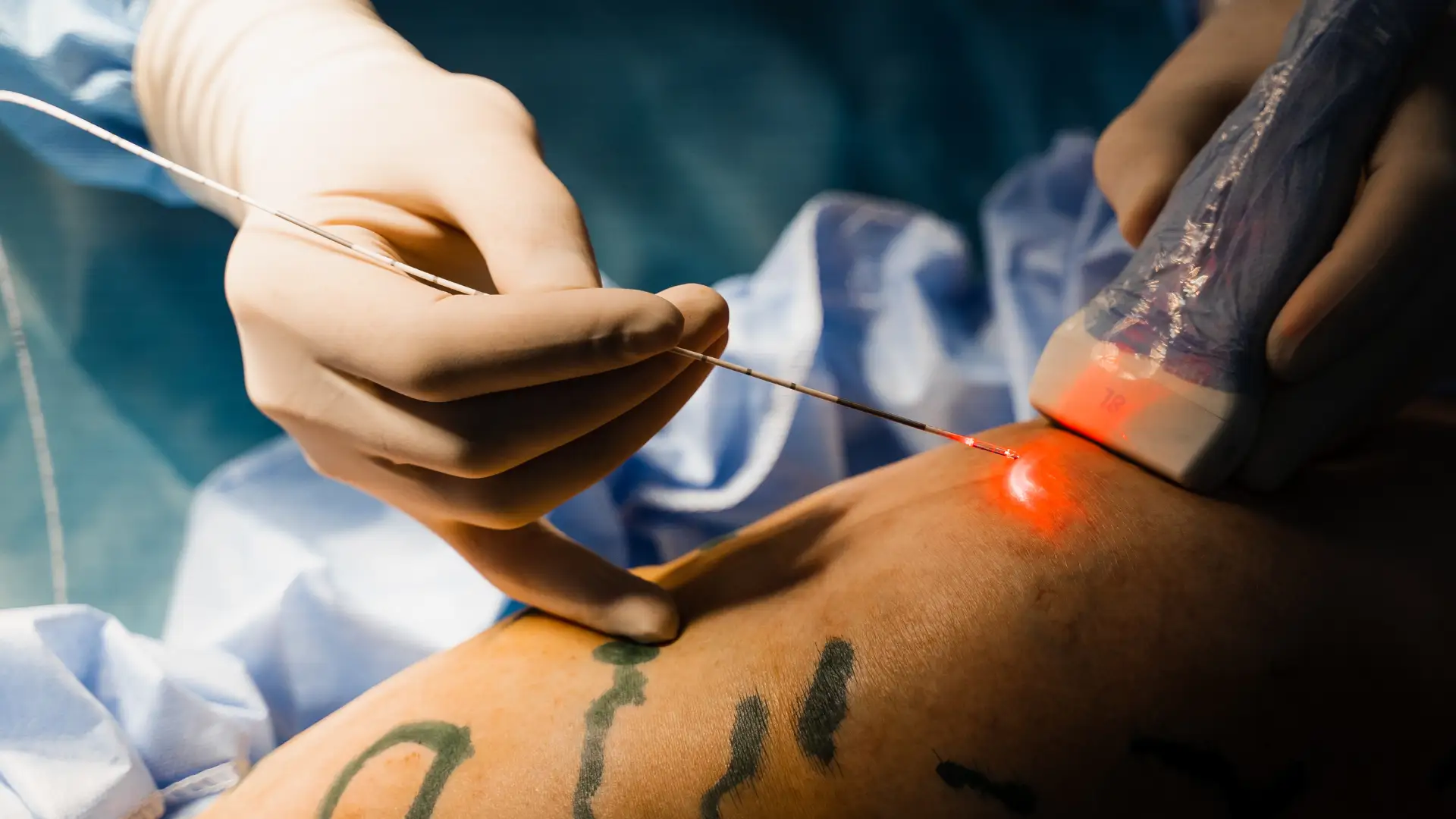
If your varicose veins cause discomfort, swelling, skin changes, or any of the symptoms mentioned earlier, consult a healthcare professional. If managed sooner, you can reduce the appearance of varicose veins with sclerotherapy, a minimally-invasive procedure that helps disappear 80% of veins in the first few weeks. For larger veins, we recommend Endovenous Laser Therapy, which has a 94% success rate over 5 years.
Reach out to your Primary Care Provider in Ontario for a referral to our specialist, Dr Lukasz Boba, at York Vascular and we’ll work to find a way to relieve your symptoms and pain.